There is a clear relationship between malocclusion and postural stability and balance, show researchers from three universities in Kraków. Therefore, when treating and diagnosing posture defects, one should approach the patient holistically instead of focusing only on the skeletal and muscular system.
The posture of our body, i.e. its characteristic arrangement and orientation in space, strongly depends on the structure, function and cooperation of muscles, fascia, skeleton and nervous system. Maintaining a stable standing position is possible thanks to the precise coordination of all these systems and continuous analysis of incoming stimuli.
For years there has been a debate in the scientific community about the importance of the craniomandibular system, including occlusal conditions, on postural stability. This topic still raises a lot of controversy because the research results are not consistent: some confirm, others refute the theory that there is a correlation between the masticatory system and posture.
Therefore, the team led by Dr. Monika Nowak from the Faculty of Medicine and Health Sciences at the Andrzej Frycz Modrzewski Krakow University decided to assess the impact of anteroposterior malocclusion on postural control and distribution of plantar pressure while standing and walking.
The scientists described their results in the International Journal of Environmental Research and Public Health (https://doi.org/10.3390/ijerph20021652).
MALOCCLUSION AND CENTRE OF GRAVITY
Malocclusions is often congenital and may result from hereditary or environmental factors. However, its causes may also include: abnormal breathing rhythm, posture defects, nail biting or bruxism. According to estimates, malocclusion affects approximately 56 percent of the population. For this reason alone, the analysis of individual defects and the accompanying disorders of the musculoskeletal system is justified.
Dr. Nowak's team took 90 healthy volunteers aged 19 to 35 for the study and divided them into three groups depending on the bite structure, and more precisely on the occlusion class, i.e. the position of contact between the upper and lower teeth. The first group consisted of people with a normal occlusion (Angle Class I), the second group - people with distal occlusion (Angle Class II), and the third - people with an anterior occlusion (Angle Class III).
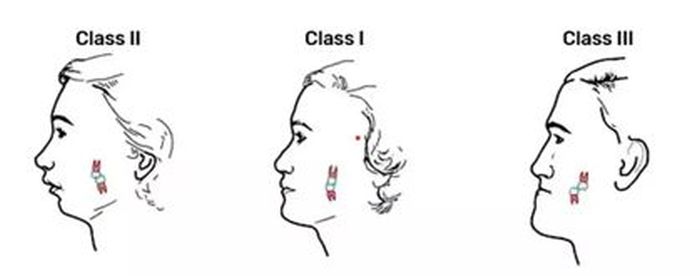
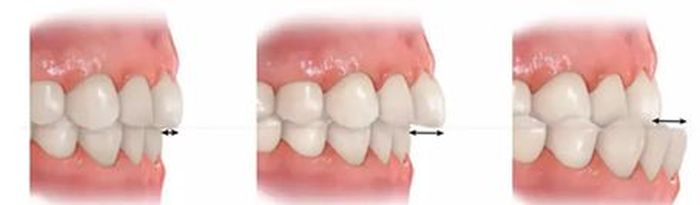
'Distal and anterior occlusion mean the relationship of the mandible to the maxilla,’ says Dr. Nowak. 'Distal occlusion is a situation in which the lower jaw and lower teeth are recessed in relation to the upper jaw and teeth, and an anterior occlusion is a situation in which the lower jaw and lower teeth are too far forward.’
The researchers then assessed participants' posture, including stability, balance, foot weight-bearing, and gait.
It turned out that there were very clear differences between people from the three research groups. For example, people with distal occlusion tended to shift the centre of foot pressure forward compared to the other groups, and both distal and anterior occlusion were associated with markedly different results of various postural tests. In a word: occlusion had an impact on the static postural stability, and patients with occlusion disorders had poorer stability and a tendency to shift the centre of gravity.
'Various areas of the body are connected through myofascial chains and neural structures,’ says Dr. Nowak. 'Therefore, any change in the stomatognathic system (e.g. malocclusion) that affects the biomechanics of the temporomandibular joint may generate changes in the tension of the masticatory muscles and the directly linked neck muscles. Then, through myofascial chains, these changes can be transmitted to other muscles, even those in the pelvis and lower limbs.’
In addition, the scientist explains, as a result of unbalanced contact of the upper and lower teeth, there is a disturbance in the reception of signals by periodontal proprioceptors, responsible for the so-called deep sensation and various muscle tensions. These abnormalities disrupt the neural information transmitted to the brain, which affects, for example: the disruption of functions of the eyeballs and the muscles of the shoulder girdle, which after the compensatory mechanisms are exhausted, affect the lower segments of the body through the muscles and fascia.
Both the discussed study and several previous studies prove that there is a link between malocclusion and postural disorders. Dentists themselves increasingly recognize the need to cooperate with physiotherapists - without this, their orthodontic treatment may not bring satisfactory results.
According to Dr. Nowak, each patient must be approached holistically instead of focusing on one system only, because our entire body is a network of interconnections. 'Orthodontic treatment can be an important part of the prevention of postural abnormalities and pain in the masticatory system and the entire musculoskeletal system, and thus prevent injuries,’ Nowak says.
She adds: ‘This is important because currently malocclusions affect up to 79 percent of Polish children. Taking care of this problem in a timely manner will significantly reduce the risk of occurrence of what I often observe in the physiotherapy office, i.e. the so-called descending disorders. This is a situation in which abnormalities in the upper parts of the body adversely affect the lower areas. Restoring stable conditions in the craniomandibular area may therefore be the beginning of restoring the synchronized functioning of the entire musculoskeletal system.
'Only an interdisciplinary cooperation of specialists contributes to the effective elimination of existing deficits.’
PAP - Science in Poland, Katarzyna Czechowicz
kap/ agt/
tr. RL















